Prior authorization comes from your insurance to verify and/or modify the prescription request sent in by your provider. The process to complete the prior authorization request can take 2-3 days.
Usually, your prescription is sent to the pharmacy by the end of your session or the end of the day. Please wait for your pharmacy to contact you and let you know when your script is ready for pickup.
Need an Rx Refill? Log into the Client Portal to notify your nurse practicioner that you need a refill.
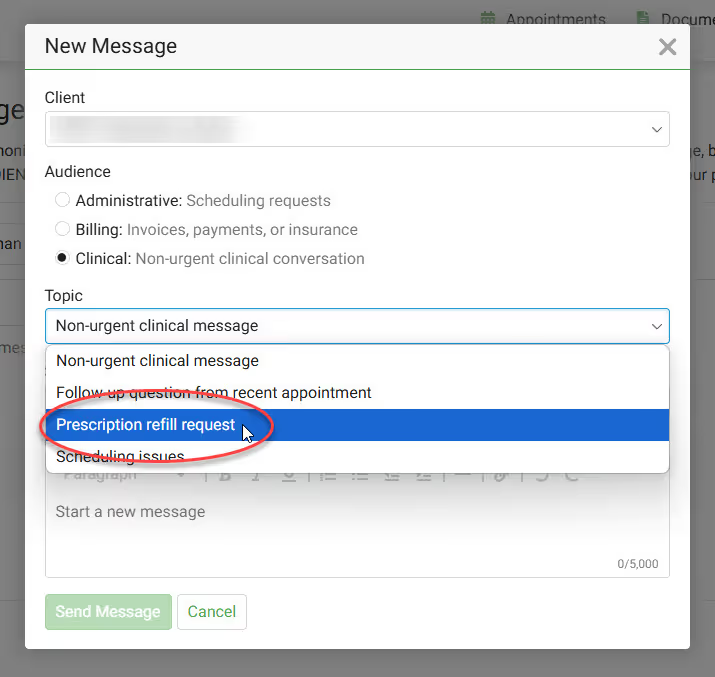
Refills of controlled substances will most often require a session with your provider. You can continue to complete the request; however, after completing the request, you can proactively take the next step and book a follow-up session with your provider.
Common controlled substances:
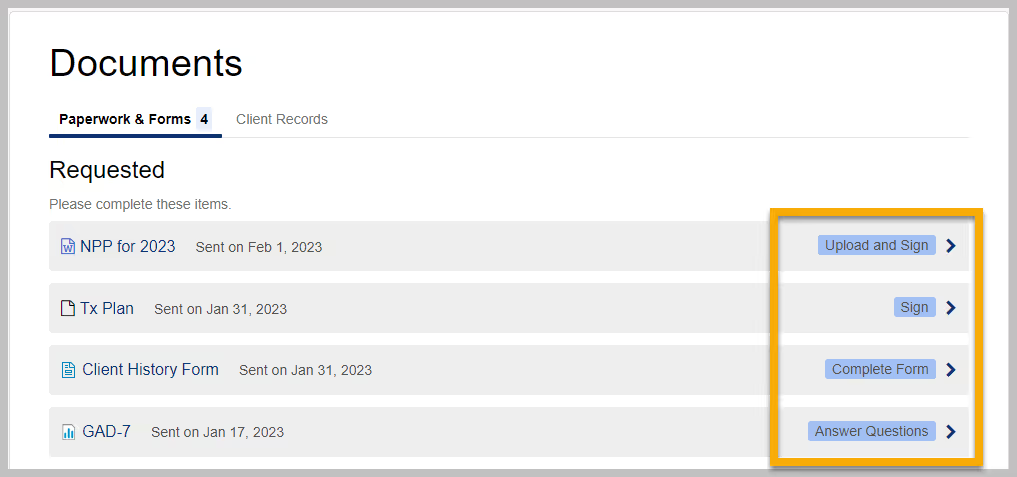
You can locate documents Overcomers' has sent you for e-sign in the Client Portal. Pending documents are shown on your homepage as well as the Documents page.
Yes, you can! In the Client Portal, you can send a message directly to your provider. Send them messages about:
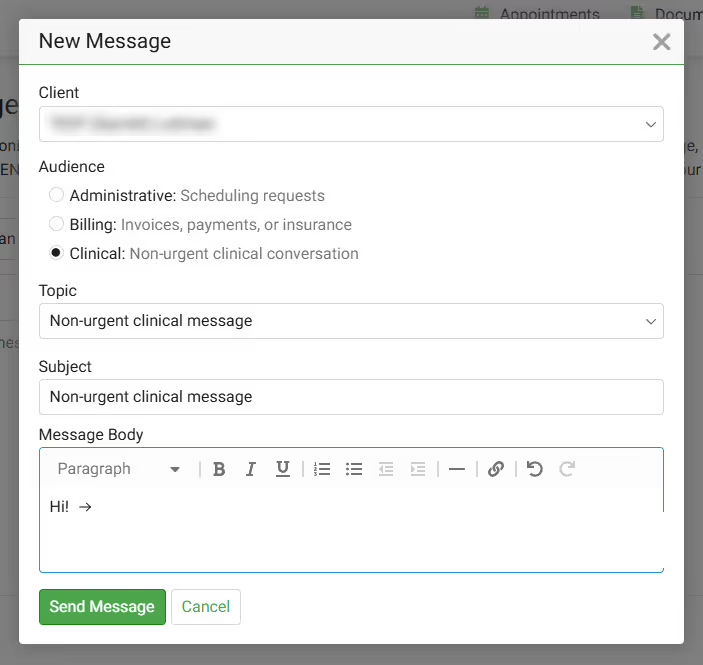
If you are unable to access the Client Portal, you can also send a message directly to your provider here.
If you have records (i.e. Medical Records) that you want to send to your provider at Overcomers, you can email them at support@overcomewithus.com. You may also visit the Client Portal, click the Documents tab and then click Upload Document.